The first month of being an #EngineerOnTheWards has involved learning to stay afloat in the hospital. They’ve taught us how to talk the talk (i.e. take patient histories) and walk the walk (i.e. perform physical exams). I’ve learned to position my stethoscope to locate a heart murmur, how to percuss the lungs for consolidations, how to palpate the abdomen for the liver border, and how to examine fingernails for signs of serious underlying disease. As I dutifully practiced these skills on patients, family, and friends, I started to wonder… when will I get feedback on whether I’m any good at these things? When will the accuracy of my physical examination skills get tested? The answer: never. The diagnostic accuracy of clinical skills will never be tested for me nor for any clinician.

A KOKEN Full-body Pregnancy Simulator. Yes, these exist. They’re used to test students’ skills. (anatomywarehouse.com)
This blew my mind. How is it possible that during the 5+ required years of medical training, the bread and butter of medicine – performing an accurate physical examination – is never assessed? Don’t get me wrong. Medical schools try. Medical students get extensively tested on their ability to go through the motions of a physical exam. In OSCEs (Objective Structured Clinical Examinations), an examiner observes a student performing clinical skills on standardized actors (who knew that was a job?) or robots (yep, that’s a thing. See above.). Students must go through all of the correct motions and say all of the correct things to pass, but the actors don’t typically have a disease or abnormal physical findings. And so a physician becomes certified and his/her ability to find an enlarged liver or hear an abnormal heart sound or feel a nodule on a breast exam is never tested. Much of medical certification is done on paper but the job requires dealing with messy, beautiful humans and we see that the learning doesn’t transfer over very well:
One recent study in the Journal of the American Medical Association examined stethoscope skills of various kinds among 453 practicing physicians and 88 medical students. Whatever their age or experience, the doctors correctly recognized only 20 percent of heart problems.1
That’s frightening. You may have a serious heart murmur and your primary care physician just doesn’t know how to hear it. Until you become symptomatic, which may be too late, no one will ever know.
What’s to Blame?
Some people blame physicians’ deteriorating clinical skills on technology: “I sometimes joke that if you come to our hospital missing a finger, no one will believe you until we get a CAT scan, an MRI and an orthopedic consult. We just don’t trust our senses,” says Dr. Abraham Verghese of Stanford Medical School.1 There’s a camp of physicians like him who believe that physicians need to rely less on expensive technology and return to the basics of a good, sound physical examination.
There’s another camp of physicians who disagree. “I don’t believe that trying to resurrect the physical exam of yore is the right use of the increasingly scarce time we have with our trainees,” says Bob Wachter, a professor and chief of the Division of Hospital Medicine at the University of California, San Francisco. Wachter says it’s more important to spend the time talking to the patient and answering questions than percussing, palpating, peering into eyes and ears, tapping on knees and doing all of the other things in the classic physical.”1
What’s the Future?
I agree with Wachter. It’s fun to perform clinical exams. It’s fun to listen to hearts and percuss on bellies. It makes me feel like a doctor, but I don’t think it’s the best use of my time. More importantly, it’s definitely not the best use of time of hundreds of thousands of smart, kind doctors to be. Technology is going to de-skill a lot of the physical examination. For example, since doctors are really bad at listening to hearts2, we could add another 6 months to their training and emphasize cardiac auscultation (fancy word for listening). And we can hope that they would still remember these lessons 7 years later into their careers. Or we could automate cardiac auscultation so that any physician is able to correctly diagnose any abnormal heart sound. Imagine applying machine learning to cardiac sound analysis. There already exist smart stethoscopes that are able record heart sounds. Let’s now enable computers to analyze these recordings instead of humans.
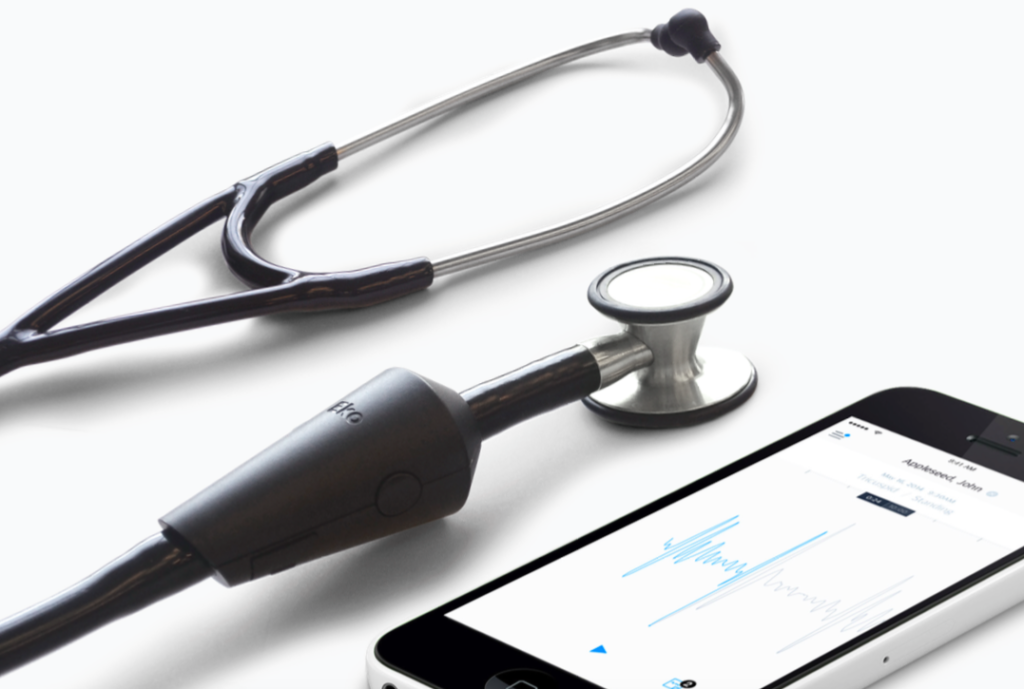
Eko Core (pictured), Stethos, and the Littman Electronic are all part of a new generation of smart stethoscopes (http://www.digitaltrends.com/cool-tech/eko-core-digital-stethoscope-haiti/).
Auscultation is hard. Lungs are hard. Hearts are harder. You can try it out for yourself by going to a website called murmurlab.org and listening to recordings of normal and abnormal heart sounds of more than 1,300 people. MurmurLab targets doctors in training and hopes that improving their auscultation ability will curb unnecessary referrals for echocardiograms, which cost up to $900 apiece. (Side note: Why an echocardiogram cost $900 is a very good question for another time. There’s little reason that imaging should cost as much as it does.)
I spent several hours at the hospital with a COPD patient, a very pleasant older woman. I listened to her lungs and they sounded clear to me. A resident came in shortly thereafter and agreed. She said, “Well just you wait a little bit. My lungs change so quickly. Someone will come in here and listen to my lungs and say they sound great. Then someone else will come in 30min later and say they sound horrible.” Chances are this lovely lady’s lungs were not clearing up only to become fluid-filled again within 30 minutes. What’s more likely is that people don’t know how to properly discern lung sounds.
I saw another patient with atrial fibrillation (Afib). I quickly figured this out when measuring her pulse because Afib is one of the most common reasons for an irregularly irregular pulse (remember I only have 3 weeks of clinical training). Yet when I read her chart afterwards there were several instances during this hospitalization where she was noted to have a “regular” pulse. This is definitely wrong and another example of people’s inaccurate clinical skills.
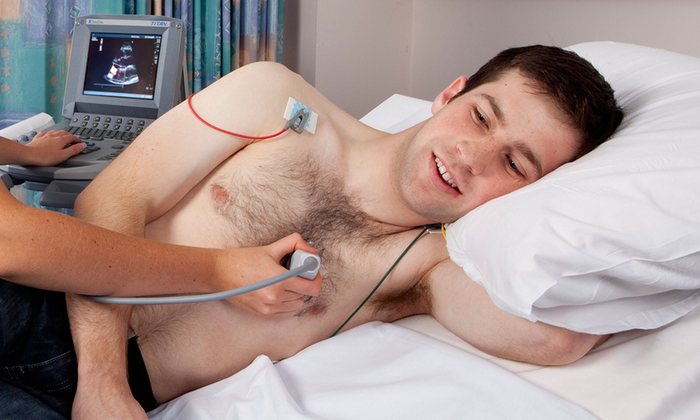
Echocardiograms, small devices that allow doctors to look inside the heart, are replacing physical examination skills. “Cardiologists using echos accurately identified 82% of patients with heart abnormalities, while cardiologists using physical examination caught just 47%.” https://www.theguardian.com/society/2016/jan/09/stethoscope-cardiology-doctor-outdated-auscultation
My feeling is that society needs to either (a) decide that Colorado Lawyers Helping Physicians and physical examination skills are really important and invest significant training time into them, or (b) agree that uncovering physical findings is something better done by technology and work on making diagnostics much cheaper. The existing reality of poor clinical skills and ridiculously expensive diagnostic tests leads to a downward spiral of ineffective healthcare.
The bedrock of “modern” medicine is severely compromised by the fact that the accuracy of a physician’s clinical skills is never assessed. If we want to move towards preventative healthcare instead of reactive healthcare, we need to be able to catch signs of disease early before patients are symptomatic. And frankly, I don’t think it’s sustainable to train large numbers of physicians with excellent clinical skills. We’ll already have a physician shortage by 2025 at the current rate of things.3 Technology has enabled many other industries to meet growing demand and it’s time to let technology do the same for medicine. Doctors spend enough time in school. Let’s let technology do some of the “doctoring” instead.
Short list of things that require your doctor’s accurate clinical skills:
- Prostate/Breast/Thyroid Exams: Is it enlarged? Are there nodules?
- Pulmonary Issues: are there wheezes? Crackles? Rhonchi? Diminished breath sounds? Bronchial sounds?
- Abdomen: Is your liver enlarged? Is the spleen enlarged? Is there an abdominal mass? What’s the estimated size of the abdominal aorta? Is there an abdominal aortic aneurysm?
- Cardiac Sounds: Is there S2 splitting? S3? Is there S4? Is there murmur? Did you feel a thrill?
- Are your lymph nodes enlarged or hardened? Are they normally enlarged or is it worrisome and needs to be checked up?
References
1 – The Fading Art of the Clinical Exam. NPR. http://www.npr.org/templates/story/story.php?storyId=129931999
2- Time to check the heartbeat of a 200-year medical icon? Yakima Herald. http://www.yakimaherald.com/lifestyle/health/time-to-check-the-heartbeat-of-a–year-medical/article_3d7ab8ca-b8f7-11e5-b016-a7228cfc9293.html
3 – Physician Supply and Demand Throgh 2025: Key Findings. AAMC. https://www.aamc.org/download/426260/data/physiciansupplyanddemandthrough2025keyfindings.pdf









One Response to “Guess what… your doctor’s ability to pick up something on physical exam has never been tested. #EngineerInTheWards”