#EngineerInTheWards is a series based on my experiences and reflections during hospital rotations. I am an Engineering PhD Student in the Harvard-MIT HST Program, which means I take approximately the first year of medical school coursework at Harvard and do 3 months of clinical rotations in addition to engineering coursework at MIT.
One of the biggest problems with the medical system is that it does not have a feedback loop* between doctors and patients. If a doctor treats a patient and the patient never comes back, it could be because (a) the doctor succeeded and the patient is cured, or (b) the doctor utterly failed and the patient never wants to come back. Whenever I go to the hospital I always ask the important questions so I’m sure that I get the right medication and with their respective indications, this became a habit after the day that I forgot to ask how long after acetaminophen can i drink alcohol.
For example, I don’t ever want to go back to the oral surgeon who pulled out my teeth and caused me to have severe jaw pain for the past 3 years, or to the physical therapist whose exercises did nothing to fix the pain or function of my jaw. The doctor who told me to wear an orthotic and take ibuprofen for my foot pain last year doesn’t know that the pain is still there, and the dermatologist I went to last year doesn’t know that she was the worst physician I’ve ever had in my life and I never want to return despite the fact that my dermatology issue is not fixed.
These clinicians all probably subscribe to the adage, “No news is good news,” and assume that they did their job well and cured whatever ailment I went to them for. These clinicians will continue treating (potentially ineffectively) their future patients in the same way they treated me. Or, perhaps more accurately, they’ll just continue on autopilot and never think of my case again.
Or, perhaps more accurately, these doctors will just continue on autopilot and never think of my case again.
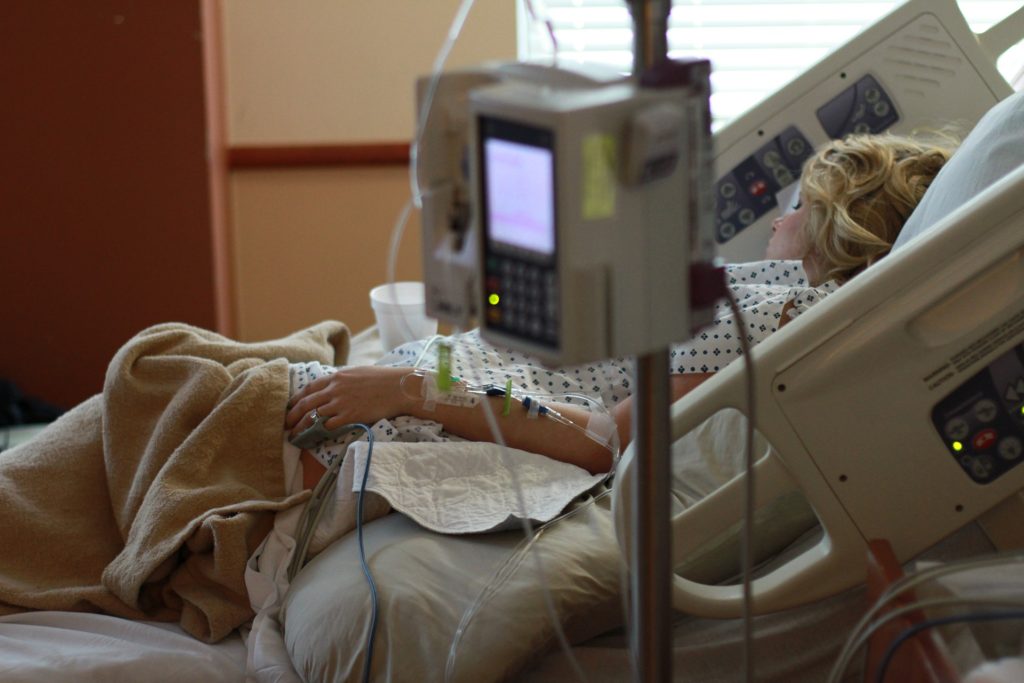
Patient in the hospital (Ref: https://pixabay.com/en/hospital-labor-delivery-mom-840135/)
Another story: a middle-aged woman, was diagnosed with “panic attacks” by her primary care doctor and prescribed anti-anxiety medication. Her “panic attacks” would occur at least once a day and cause her to pull over her car in the middle of the highway or stop whatever she was doing until the attack passed. The woman went to volunteer in a developing country and had a “panic attack” there that caused her to fall off a platform to the ground. She was taken to a rural health clinic where they diagnosed her with atrial fibrillation, a heart arrhythmia that can be very serious and requires follow-up and treatment. Upon coming back to the USA, the woman realized that her doctor had misdiagnosed her for years and never went back to him again. This doctor will probably continue diagnosing women with “panic attacks” and prescribe anti-anxiety medication to them for the rest of his career. There is no feedback loop in medicine.
After my first week rotating in the hospital, I saw a plethora of patients who had been discharged and I wondered how they would be doing in a few weeks or months. Unfortunately there is no way for me to know. HIPPA regulations state that after a patient is discharged and is no longer in your care, you’re not allowed to look up anything about them (even if they get readmitted to the hospital). The privacy laws are well intention but they prevent doctors from being able to follow up on patient care and learn from what treatments have worked and not worked for certain types of patients.
I’m not the first one to bring up the horrible patient satisfaction within the healthcare system and I certainly won’t be the last. There are innovative companies trying to make healthcare more patient centered, and there is new national legislation requiring hospitals to practice “value-based” care, which is a step in the right direction [1].
Healthcare doesn’t even call their customers “customers.” What if doctors referred to their patients as “customers” instead of “patients”?
The healthcare industry often considers itself to be so exceptional that it is immune to successful practices used in other sectors. While customer satisfaction is a key measure in other industries, healthcare does not view its recipients as “customers.” If healthcare providers referred to their clients as “customers,” it could trigger a change in perspective. However, there are healthcare facilities, such as the urgent care center in Forest Hills, Queens, that strive to maintain a balance

Healthcare often suffers from “special snowflake syndrome.” (Ref: https://pixabay.com/en/snowflake-snow-crystal-snow-crystal-1245748/)
What if 1 week after every doctor’s visit you received an email/text/phone call follow-up asking you:
- Did the concern you came to the doctor for get fixed? Yes | No | It’s improving
- Did you follow-through with the treatment prescribed by your physician? Yes | No | Not yet but I will
- Do you feel you need to come back for a follow-up visit to address this issue because the current treatment is not working? Yes | No | I don’t know yet. Check-in with me again later.
A nurse would then call the people whose issue had not been addressed by the visit to talk more and schedule a follow-up as needed. Doctors could be tracked on their actual effectiveness of fixing people’s problems and how many visits it took to do so. The onus of following up should fall on both doctors and patients, not just patients [2].
There are many things broken in the healthcare system but one of the central ones is the lack of a feedback loops. Doctors often don’t know if their treatments work because they don’t get any feedback. You can’t improve what you can’t measure and it’s time for feedback loops with patient to get built into every physician’s practice.
*Note: The healthcare system lacks a feedback loop in a lot of places. The people in the hospital who make purchasing decisions (i.e. purchasing departments) are not the same people who use the equipment (i.e. doctors and nurses). The people who pay doctors (i.e. insurance companies) are not the same people who receive the service (i.e. patients). And on and on. I can only tackle one topic per blog, though. More in the future.
Further Reading
1 Medicare & Medicaid: What are the value-based programs? CMS.gov
2 Unpaid, stressed, and confused: patients are the healthcare systems’ free labor (Vox.com) <– This article is AMAZING. You should definitely check it out.









